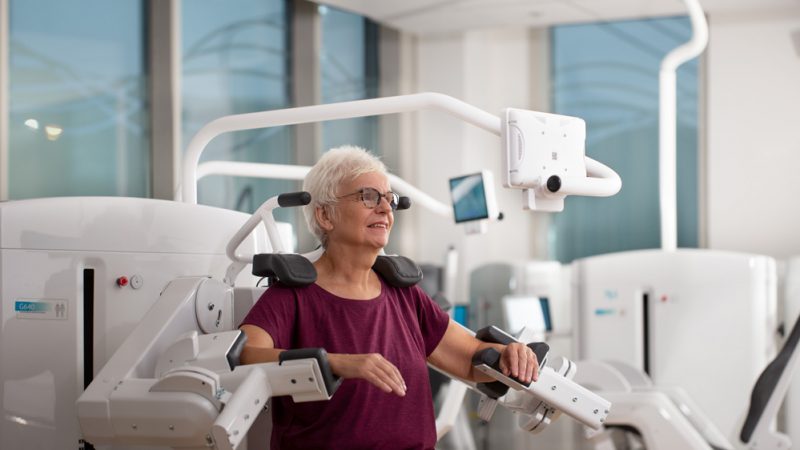
The Cost Crisis That Changed Everything
Healthcare systems worldwide face an unsustainable trajectory. Chronic musculoskeletal conditions alone cost the U.S. economy over $980 billion annually when accounting for direct medical expenses and lost productivity. Traditional treatment models relying heavily on pharmaceuticals, injections, and surgical interventions, have delivered disappointing results while driving costs ever higher.
Insurers have recognized a stark reality: the status quo isn’t working. They’re paying enormous sums for treatments that often fail to address root causes, leading to recurring claims, prolonged disability, and diminished quality of life for patients. This realization has opened the door to evidence-based alternatives that can demonstrate measurable outcomes.
What Makes Device-Based Exercise Therapy Different?
Not all exercise is created equal, and insurers understand this distinction. Device-based exercise therapy offers several characteristics that traditional approaches lack: Standardization and reproducibility. Medical-grade exercise equipment provides consistent resistance, controlled range of motion, and repeatable protocols. This standardization means that outcomes achieved in clinical trials can be reliably replicated in real-world settings—a critical factor for evidence-based medicine.
Objective measurement and data collection. Modern exercise therapy devices capture detailed performance metrics: force production, range of motion, pain levels, and functional improvements. This data enables providers to track progress objectively and adjust treatment protocols based on measurable outcomes rather than subjective impressions. Targeted intervention for specific conditions. Unlike general fitness programs, device-based therapy allows precise targeting of affected muscle groups and joints. For conditions like chronic low back pain, cervical disorders, or post-surgical rehabilitation, this specificity translates to superior outcomes. Reduced need for costly alternatives. When exercise therapy effectively manages a condition, it often prevents or delays more expensive interventions. Avoiding a single spinal fusion surgery, which can cost $80,000 to $150,000, provides substantial return on investment. Reduced need for costly alternatives
Effective exercise therapy can prevent or delay expensive interventions. Avoiding procedures such as spinal fusion surgery (costing €80,000–€150,000) can deliver a substantial return on investment. However, in some cases, surgery cannot be ruled out, and this will always depend on the individual patient and clinical situation.
The Evidence Base Has Reached Critical Mass
Insurers operate on evidence, and the research supporting device-based exercise therapy has become impossible to ignore. High-quality studies have demonstrated effectiveness across multiple conditions: Chronic low back pain patients using device-based strengthening programs show significant improvements in pain, function, and return to work rates compared to conventional physical therapy. Studies report pain reductions of 40-60% and functional improvements that persist for years after treatment completion. For neck pain and cervical disorders, targeted strengthening of cervical musculature using specialized equipment has shown superior outcomes to manual therapy or general exercise, with some studies reporting 70-80% of patients achieving clinically significant improvement.
Post-surgical rehabilitation programs incorporating device-based protocols demonstrate faster recovery times, better functional outcomes, and lower re-operation rates compared to standard care. This evidence is particularly compelling for orthopedic procedures where rehabilitation quality directly impacts surgical success.
Osteoarthritis management through controlled, progressive resistance training has proven effective at reducing pain, improving function, and potentially slowing disease progression, outcomes that matter both clinically and economically.

Source: Siwa Clinic, Spain.
Value-Based Care Alignment
The shift toward value-based payment models has accelerated insurer interest in device-based exercise therapy. Under fee-for-service models, there was little incentive to invest in interventions that might reduce future claims. Value-based arrangements flip this logic, rewarding providers for keeping patients healthy and functional. Device-based exercise therapy aligns perfectly with value-based metrics. It addresses the underlying cause of many musculoskeletal conditions—muscular weakness and dysfunction—rather than merely treating symptoms. This approach reduces long-term healthcare utilization, improves patient-reported outcomes, and enhances quality-adjusted life years (QALYs), all key metrics in value-based contracts.
Accountable care organizations and bundled payment programs have been early adopters, recognizing that investing in effective exercise therapy reduces downstream costs and improves population health metrics.
The Technology Advantage
Modern device-based exercise therapy leverages technology in ways that address traditional barriers to reimbursement:
Telehealth integration allows patients to receive supervised therapy remotely, expanding access while reducing overhead costs. Insurers value this efficiency, particularly for patients in rural areas or those with mobility limitations. Automated documentation integrated into exercise devices streamlines the administrative burden, ensuring that sessions are properly documented for billing and compliance. This reduces friction in the reimbursement process. Predictive analytics using machine learning can identify patients at risk of non-compliance or poor outcomes, enabling early intervention. Insurers appreciate this proactive approach to managing their populations. Patient engagement tools built into modern platforms improve adherence rates, which directly correlates with better outcomes. When patients complete their prescribed therapy, insurers see the results in reduced claims.
Real-World Outcomes That Matter
Beyond controlled clinical trials, real-world evidence from healthcare systems implementing device-based exercise therapy has been compelling. Several large integrated delivery networks have reported:
- 30-50% reductions in opioid prescriptions for chronic pain patients
- 40% decreases in advanced imaging utilization for low back pain25-35% reductions in surgical referrals for conditions amenable to conservative care
- Significant improvements in patient satisfaction scores
- Reduced disability duration and faster return to work
These outcomes translate directly to cost savings. When a major U.S. health system implemented a comprehensive device-based exercise therapy program for musculoskeletal conditions, they documented a 3:1 return on investment within the first year, with savings increasing in subsequent years as preventive benefits accumulated.
Regulatory and Professional Recognition
Reimbursement decisions don’t happen in a vacuum. The growing acceptance of device-based exercise therapy reflects broader professional and regulatory endorsement: Major clinical practice guidelines now include therapeutic exercise as a first-line recommendation for conditions like chronic low back pain, osteoarthritis, and many post-surgical scenarios. When respected professional organizations endorse an intervention, insurers take notice.
Medicare and Medicaid programs in various jurisdictions have established specific billing codes and coverage policies for medically supervised exercise therapy, creating a template that private insurers often follow.
Occupational health and workers‘ compensation systems have been particularly enthusiastic adopters, recognizing the rapid return-to-work benefits and reduced permanent disability rates associated with structured exercise therapy programs.
The Prevention Paradigm
Perhaps the most forward-thinking insurers recognize device-based exercise therapy’s potential for primary and secondary prevention. By identifying at-risk individuals and intervening before conditions become chronic and costly, healthcare systems can fundamentally alter disease trajectories.
Worksite wellness programs incorporating device-based screening and preventive exercise have demonstrated reductions in musculoskeletal injury rates and associated claims. While still emerging, this application represents potentially enormous value for insurers covering large employer groups.
Challenges Remain, But Momentum Is Clear
Despite growing acceptance, barriers to universal reimbursement persist. Coverage policies vary widely between insurers and geographic regions. Prior authorization requirements can create administrative hurdles. Some insurers still struggle to differentiate medically necessary therapy from general fitness programs.
Education remains crucial, both for payers who may not understand the evidence base and for providers who need to document medical necessity appropriately. Standardized outcome measures and quality reporting will likely accelerate acceptance.
Looking Forward
The trend toward reimbursement for device-based exercise therapy reflects a broader maturation of healthcare economics. Insurers are increasingly sophisticated in evaluating interventions based on long-term value rather than short-term costs. They recognize that paying for effective conservative care often prevents expensive downstream interventions.
For manufacturers and providers of device-based exercise therapy, this evolution creates both opportunity and responsibility. The opportunity lies in growing market access and the ability to help more patients. The responsibility involves maintaining rigorous outcome measurement, continual quality improvement, and transparent communication of results.
As healthcare continues its shift toward value-based models, interventions that combine strong clinical evidence, measurable outcomes, and cost-effectiveness will flourish. Device-based exercise therapy checks all these boxes, explaining why insurers are increasingly willing to reimburse for this approach.
The message is clear: exercise therapy has evolved from a nice-to-have adjunct to an evidence-based, economically justified intervention that belongs in mainstream healthcare. For patients suffering from musculoskeletal conditions, this shift opens doors to effective treatment. For healthcare systems, it offers a sustainable path forward. And for insurers, it represents smart investment in the health of their populations.
DAVID Health is at the forefront of device-based exercise therapy, providing evidence-based solutions that improve patient outcomes while reducing healthcare costs. Our medical-grade equipment and comprehensive therapy protocols are designed to meet the highest standards of clinical effectiveness and reimbursement compliance.
 Deutsch
Deutsch