What Is Adhesive Capsulitis?
Adhesive capsulitis, commonly called frozen shoulder, is a condition characterised by painful, progressive restriction of both active and passive glenohumeral joint range of motion, without a clearly identifiable intrinsic shoulder disorder. The hallmark is restriction in all planes, particularly external rotation, which distinguishes it from rotator cuff pathology or subacromial impingement.
The underlying mechanism involves fibrosis of the glenohumeral joint capsule. Chronic inflammation triggers the formation of thick bands of scar tissue (adhesions), the capsule thickens and contracts, and synovial fluid production is reduced, progressively limiting the joint’s ability to move and rotate. Emerging research also points to a role of pathological motor control and ‘muscle guarding’, suggesting the restriction is not purely mechanical but also involves aberrant neuromuscular recruitment patterns.
Classification
- Primary (idiopathic); occurs without a known trigger; strongly associated with endocrine disorders such as type 2 diabetes and thyroid dysfunction.
- Secondary; develops after a known event such as rotator cuff injury, shoulder surgery, fracture, or prolonged immobilisation.
| Age 40–65
Peak incidence in middle age; uncommon under 40 |
Female sex
Women are affected more often than men |
| Diabetes mellitus
10–36% prevalence vs. 2–5% in general population |
Thyroid disorders
Both hypo- and hyperthyroidism elevate risk |
| Shoulder injury/surgery
Immobilisation is a key secondary trigger |
Neurological conditions
Parkinson’s disease and stroke increase risk |
The Three Clinical Stages
Adhesive capsulitis progresses through three well-defined stages. Recovery is largely self-limiting, but the total trajectory spans anywhere from 12 months to over 3 years, and up to 40% of patients report persistent symptoms beyond three years without structured intervention. Early identification and stage-appropriate treatment are essential to reduce this burden.
| FREEZING | FROZEN | THAWING |
| 6 weeks – 9 months | 4 – 12 months | 6 months – 2+ years |
Stage 1
The Freezing Phase — « Painful »
Duration: 6 weeks to 9 months
This is the most acutely painful phase. Patients describe a gradual, insidious onset of diffuse, deep shoulder aching that is characteristically worse at night and disrupts sleep. The pain typically begins without a specific precipitating event and is often mistakenly attributed to rotator cuff tendinopathy in the early weeks.
- Gradual onset of shoulder pain, increasing in intensity over weeks
- Significant night pain; often unable to lie on the affected side
- Progressive loss of active and passive range of motion in all planes
- External rotation is typically the first and most restricted movement
- Pain at rest, worsening sharply at end range
Stage 2
The Frozen Phase — « Stiff »
Duration: 4 to 12 months
Pain gradually subsides, though it remains at extremes of movement, while stiffness becomes the dominant clinical feature. Patients often report a paradoxical sense that the shoulder is ‘getting better’ because the constant pain has eased, yet functional disability remains severe.
- Marked reduction in all glenohumeral movement planes (capsular pattern)
- Pain primarily provoked at end range; less pain at rest
- Progressive difficulty with overhead tasks, behind-back movements
- Compensatory scapulothoracic movement becomes prominent
- Muscle disuse and strength deficits begin to accumulate
Stage 3
The Thawing Phase — « Recovery »
Duration: 6 months to 2+ years
Spontaneous, progressive improvement in range of motion characterises this phase, with minimal pain. However, muscle strength and neuromuscular coordination remain significantly impaired even as joint mobility returns, making this phase the critical window for targeted strengthening and motor control restoration.
- Gradual return of glenohumeral range of motion
- Minimal pain at rest; mild discomfort at extreme end ranges
- Persistent rotator cuff and scapular stabiliser weakness
- Abnormal muscle recruitment patterns require active correction
- Full or near-full recovery possible with structured exercise therapy
Treatment Principles: Why Exercise Therapy Leads
The evidence base consistently positions physical therapy as the primary first-line treatment for adhesive capsulitis. While pharmacological interventions (NSAIDs, oral glucocorticoids) and corticosteroid injections play a role, particularly in Stage 1 for pain control, they do not address the underlying muscular weakness and abnormal motor control that perpetuate disability.
Early corticosteroid injection within the first six months has been shown to reduce the duration of the freezing phase by three to six months compared to conservative management alone. However, when conservative methods are combined with structured exercise, outcomes are consistently superior to either approach in isolation.
What the Evidence Shows
Posterior glenohumeral mobilisation has demonstrated the largest effect size for improving range of motion. High-grade mobilisation techniques (Maitland Grades III–IV) significantly improve ROM in patients with frozen shoulder of at least three months’ duration.
Rotator cuff strengthening combined with motor control training shows moderate to strong benefit, particularly important in the thawing phase, where strength deficits outlast pain by months.
Studies demonstrate that prompt, structured intervention can reduce total recovery time from 30–36 months down to 18–24 months. Patients who wait passively risk permanent mobility restrictions and chronic pain patterns.
The rehabilitation approach should be tailored to stage. In the freezing phase, the priority is pain management and gentle mobility work. In the frozen phase, progressive joint mobilisation and patient education take centre stage. In the thawing phase, the focus shifts decisively toward measurable, progressive strengthening of the rotator cuff and scapular stabilisers, precisely where device-based exercise therapy delivers its greatest advantage.
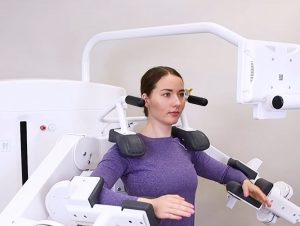
Precision Shoulder Rehabilitation with DAVID
The DAVID Shoulder Solution was designed specifically for the rehabilitation challenges conventional shoulder devices fail to address. Standard fitness equipment targets the large prime movers of the upper body, but shoulder pain, including frozen shoulder, primarily stems from dysfunction in the small rotator cuff muscles and scapular stabilisers: structures that standard equipment cannot effectively isolate.
DAVID’s biomechanical engineering resolves this. Each device uses joint-specific isolation, scientifically validated resistance curves aligned to the muscle’s strength-length relationship, and precise axis alignment, enabling safe, targeted loading of the rotator cuff from the earliest stages of rehabilitation.
| DAVID Health Solutions · Key Capabilities | |
| 1 | Rotator Cuff Isolation
Precisely targets internal and external rotators and scapular stabilisers that conventional equipment cannot reach. |
| 2 | Quantified Exercise
Every session logs ROM, load, speed, and range progression automatically, turning subjective progress into objective clinical data. |
| 3 | EVE Software
A protocol generation and adaptive loading progression based on real-time biofeedback and mobility test results. |
| 4 | Pain-Free Loading
Natural resistance curves allow safe joint loading without harmful strain, critical for pain-sensitive frozen shoulder patients. |
The DAVID Shoulder Devices in Practice
The DAVID Shoulder Solution comprises a purpose-built set of devices that together address the full spectrum of shoulder dysfunction, from acute rotator cuff isolation in restricted ranges to progressive scapular stabilisation in the return-to-function phase.
Matching DAVID Rehabilitation to the Clinical Stage
A key advantage of the DAVID system is its ability to precisely match treatment parameters, load, ROM, speed, set/rep volume, to the patient’s current clinical stage.
| Stage | Primary Goal | DAVID Application | EVE Software Role |
| Stage 1 · Freezing | Pain reduction; maintain available ROM; prevent further capsular restriction | Very low load, narrow pain-free ROM arcs; isometric testing as baseline; gentle rotator cuff activation | Sets conservative ROM limits; flags pain responses; collects baseline mobility data |
| Stage 2 · Frozen | Progressive ROM restoration; prevent muscle atrophy; patient self-management | Graduated load progression; ROM limits expanded incrementally per test results; all shoulder devices introduced | Diagnosed Based-generated protocol progression; automated load increases; compliance tracking; outcome reporting |
| Stage 3 · Thawing | Full strength restoration; motor control; return to normal function and ADLs | Full programme with progressive overload; scapular stabilisation emphasis; high-rep endurance phases | Comparative outcome reporting; patient satisfaction tracking; programme graduation criteria |
The EVE Platform: Making Rehabilitation Measurable
One of the most clinically significant differentiators of the DAVID system is the EVE software platform, a cloud-based SaaS solution that transforms exercise therapy from a qualitative intervention into a quantified, data-driven clinical process.
For frozen shoulder specifically, this matters enormously. Clinicians can objectively track how many degrees of external rotation the patient has gained this week, whether the load-to-pain ratio is improving, and whether ROM limits can be safely advanced, all from automated data collected during every session without additional administrative burden.
The EVE system also manages patient intake (automated digital forms), generates training programmes based on mobility and isometric test results, guides patients through sessions via colour-coded visual terminals, and produces outcome reports for clinical audit, insurance documentation, and quality benchmarking.
For a condition as variable and prolonged as adhesive capsulitis, where patient expectations must be carefully managed across a 12–36 month recovery, the ability to show patients objective, graphed progress data over time is a powerful motivational and therapeutic tool in itself.
Summary: Key Clinical Takeaways
Adhesive capsulitis is a self-limiting but potentially prolonged and debilitating condition. The three-stage model, freezing, frozen, thawing, provides a clinically useful framework for matching treatment intensity and focus to the patient’s current presentation. Early diagnosis and structured intervention, led by exercise therapy, consistently outperform watchful waiting.
The DAVID Shoulder Solution addresses the core rehabilitation challenge of frozen shoulder: the need to safely load the rotator cuff and scapular stabilisers in a restricted, pain-sensitive joint, with precise, measurable, and progressively advancing parameters. By combining biomechanically optimised devices with the EVE software platform, clinicians can deliver a rehabilitation programme that is not only clinically superior, but also efficient, scalable, and objectively documented.
Ready to Deliver Measurable Shoulder Rehabilitation?
Learn how the DAVID Shoulder Solution is helping physiotherapy practices and rehabilitation centres across 40+ countries transform shoulder care outcomes.
Visit: davidhealth.com/device-based-solution/shoulder/
Clinical Disclaimer: This article is intended for healthcare professionals and is provided for educational purposes only. It does not constitute medical advice. The management of adhesive capsulitis should be tailored to the individual patient’s clinical presentation, comorbidities, and response to treatment. Always consult current clinical guidelines and exercise clinical judgement.
1. Clinical Guidelines & Orthopaedic References
- American Academy of Orthopaedic Surgeons (AAOS). (2022). Frozen shoulder (adhesive capsulitis). https://orthoinfo.aaos.org/en/diseases–conditions/frozen-shoulder
- Cleveland Clinic. (2024, January 30). Frozen shoulder (adhesive capsulitis): Symptoms & treatment. Cleveland Clinic Health Library. https://my.clevelandclinic.org/health/diseases/frozen-shoulder-adhesive-capsulitis
- Mayo Clinic. (2022). Frozen shoulder — Symptoms and causes. https://www.mayoclinic.org/diseases-conditions/frozen-shoulder/symptoms-causes/syc-20372684
- St George’s Shoulder Unit (SGSU). (2024). Adhesive capsulitis (frozen shoulder): Patient information leaflet. St George’s University Hospitals NHS Foundation Trust. https://www.stgeorges.nhs.uk/wp-content/uploads/2024/10/PHY_FSAC.pdf
- Brigham and Women’s Hospital, Department of Rehabilitation Services. (2010). Standard of care: Adhesive capsulitis. https://www.brighamandwomens.org/assets/BWH/patients-and-families/rehabilitation-services/pdfs/shoulder-adhesive-capsulitis.pdf
2. Peer-Reviewed Scientific Literature
- Challoumas, D., Biddle, M., McLean, M., & Millar, N. L. (2020). Comparison of treatments for frozen shoulder: A systematic review and meta-analysis. JAMA Network Open, 3(12), e2029581. https://doi.org/10.1001/jamanetworkopen.2020.29581
- Dyer, B. P., Thomas, M. J., & Burton, C. (2023). Incidence, prevalence and risk factors for frozen shoulder: A protocol for a systematic review. BMJ Open, 13(3), e063718. https://doi.org/10.1136/bmjopen-2022-063718
- Hanchard, N. C. A., Goodchild, L., Thompson, J., O’Brien, T., Davison, D., & Richardson, C. (2011). Evidence-based clinical guidelines for the diagnosis, assessment and physiotherapy management of contracted (frozen) shoulder. Physiotherapy, 97(4), 296–310. https://doi.org/10.1016/j.physio.2011.01.001
- Prestgaard, T. A. (2023). Frozen shoulder (adhesive capsulitis). National Center for Biotechnology Information (NCBI). https://www.ncbi.nlm.nih.gov/books/NBK532955/
- Rangan, A., Hanchard, N., & McDaid, C. (2016). What is the most effective treatment for frozen shoulder? BMJ, 354, i4162. https://doi.org/10.1136/bmj.i4162
- Tanaka, K., Saura, R., Takahashi, N., & Hiura, Y. (2010). Joint mobilisation versus self-exercises for limited glenohumeral joint mobility: Randomised controlled study in patients with frozen shoulder. Journal of Rehabilitation Medicine, 42(4), 339–344. https://doi.org/10.2340/16501977-0534
- Vermeulen, H. M., Rozing, P. M., Obermann, W. R., le Cessie, S., & Vliet Vlieland, T. P. M. (2006). Comparison of high-grade and low-grade mobilization techniques in the management of adhesive capsulitis of the shoulder: Randomized controlled trial. Physical Therapy, 86(3), 355–368. https://doi.org/10.1093/ptj/86.3.355
- Wang, W., Shi, M., Zhou, C., Shi, Z., Cai, X., Lin, T., & Yan, H. (2017). Effectiveness of corticosteroid injections in adhesive capsulitis of the shoulder: A meta-analysis. Medicine, 96(28), e7529. https://doi.org/10.1097/MD.0000000000007529
3. Physiotherapy & Rehabilitation Sciences
- Favejee, M. M., Huisstede, B. M. A., & Koes, B. W. (2011). Frozen shoulder: The effectiveness of conservative and surgical interventions — Systematic review. British Journal of Sports Medicine, 45(1), 49–56. https://doi.org/10.1136/bjsm.2010.071431
- Physiopedia Contributors. (n.d.). Frozen shoulder. Retrieved March 27, 2026, from https://www.physio-pedia.com/Frozen_Shoulder
- Sivashanker, R., & Ibrahim, M. (2018). Physical therapy in the management of frozen shoulder. Singapore Medical Journal, 59(12), 649–654. https://pmc.ncbi.nlm.nih.gov/articles/PMC5917053/
- Wikipedia Contributors. (2026, March 25). Adhesive capsulitis of the shoulder. https://en.wikipedia.org/wiki/Adhesive_capsulitis_of_the_shoulder
 Français
Français 
























